In February, Telehealth Utilization Overall
Increased Nationally and in Midwest and West, but Fell in Northeast
and South, according to FAIR Health's Monthly
Telehealth Regional Tracker
Nationally and in Every Region, the Median
Allowed Amount for a 45-Minute Psychotherapy Visit Was Higher via
Telehealth Than in an Office Setting
NEW
YORK, May 15, 2024 /PRNewswire/ -- In
February 2024, mental health
conditions continued as the top telehealth diagnostic category
nationally and in every region, and grew as a percentage of
telehealth claim lines nationally and in every region, according to
FAIR Health's Monthly Telehealth Regional
Tracker.1 Nationally, mental health conditions rose
from 66.3 percent of telehealth claim lines in January to 67.2
percent in February. Regionally, the largest increase was in the
South (increasing from 56.0 percent to 57.1 percent), while the
smallest increase was in the Midwest (from 72.3 percent to 72.5
percent). The data represent the privately insured population,
excluding Medicare Fee-for-Service, Medicare Advantage and
Medicaid. These findings follow the release of FAIR Health's mental
health white paper in late April: Trends in Mental Health
Conditions: An Analysis of Private Healthcare Claims.
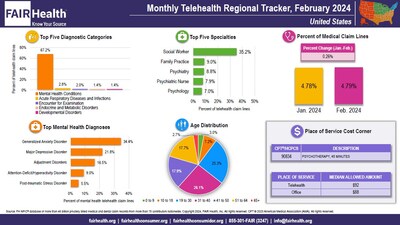
COVID-19 was not in the top five diagnostic categories
nationally or in any region in February
2024. In January, it had been ranked fourth in the
Northeast.
Mental Health Diagnoses
Generalized anxiety disorder
remained the top mental health telehealth diagnosis nationally and
in every region. In February, it accounted for more than 30 percent
of mental health telehealth claim lines everywhere. The largest
share was still in the Northeast at 38.4 percent, up from 38.1
percent in January.
Nationally and in all four census regions, the top five mental
health diagnoses in February were identical to each other:
generalized anxiety disorder, major depressive disorder, adjustment
disorders, attention-deficit/hyperactivity disorder and
post-traumatic stress disorder (PTSD). In the South, bipolar
disorder had ranked at number five in January, but in February,
PTSD filled that position, matching the other regions and the
national ranking.
Utilization
In February
2024, overall telehealth utilization increased nationally
and in the Midwest and West, but fell in the Northeast and South.
Nationally, medical claim lines associated with telehealth rose
slightly from 4.78 percent in January to 4.79 percent in February,
a 0.3 percent increase. In the Midwest, the share of claim lines
rose 2.3 percent, while in the West it rose 3.0 percent. In the
Northeast, however, there was a decrease of 4.1 percent, and in the
South, a decrease of 1.2 percent.
Specialties
In February, as in January, social worker
was the top telehealth provider specialty nationally and in all
regions. At the national level, social worker accounted for 35.2
percent of telehealth claim lines. Across regions, it varied from
29.3 percent in the South to 42.1 percent in the Midwest.
Nationally, and in the South and West, family practice remained
in the top five specialties in February. Family practice still did
not rank among the top five in the Northeast or Midwest.
Age
In February, as in January, the age group 31 to 40
accounted for the largest share of telehealth claim lines
nationally and in the South and West, while the age group 19 to 30
accounted for the largest share in the Midwest and Northeast.
The percentage of telehealth claim lines associated with each
age group varied from January to February
2024. The largest change was in the age group 0 to 9 at the
national level, which increased in its share of telehealth claim
lines by 17.9 percent (rising from 2.6 percent to 3.0 percent).
Costs
Nationally and in every region, the median
allowed amount2 for CPT®3 90834
(psychotherapy, 45 minutes) in February was higher when rendered
via telehealth than in an office. Nationally and in the Northeast,
the cost was $92 via telehealth and
$88 in an office; in the South, it
was $85 via telehealth and
$77 in an office. In the Midwest, the
cost was $93 via telehealth and
$82 in an office, and in the West,
the cost was $105 via telehealth and
$93 in an office.
About the Monthly Telehealth Regional Tracker
Launched
in May 2020 as a free service, the
Monthly Telehealth Regional Tracker uses FAIR Health data to track
how telehealth is evolving from month to month. An interactive map
of the four US census regions allows the user to view an
infographic on telehealth in a specific month in the nation as a
whole or in individual regions. Each year, the infographic
introduces varied views into telehealth utilization. In this fifth
iteration of the Monthly Telehealth Regional Tracker, each
infographic shows month-to-month changes in volume of telehealth
claim lines; that month's top five diagnostic categories, mental
health diagnoses and specialties; age distribution; and the Place
of Service Cost Corner, which compares median allowed amounts for a
specific procedure provided via telehealth to the same procedure
provided in an office;.
FAIR Health President Robin
Gelburd stated: "We are happy to share these varying windows
into telehealth utilization as it continues to evolve. This is one
of the many ways we pursue our healthcare transparency
mission."
For the Monthly Telehealth Regional Tracker, click here.
Follow us on X @FAIRHealth
About FAIR Health
FAIR Health is a national,
independent nonprofit organization that qualifies as a public
charity under section 501(c)(3) of the federal tax code. It is
dedicated to bringing transparency to healthcare costs and health
insurance information through data products, consumer resources and
health systems research support. FAIR Health possesses the nation's
largest collection of private healthcare claims data, which
includes over 46 billion claim records and is growing at a rate of
over 3 billion claim records a year. FAIR Health licenses its
privately billed data and data products—including benchmark
modules, data visualizations, custom analytics and market
indices—to commercial insurers and self-insurers, employers,
providers, hospitals and healthcare systems, government agencies,
researchers and others. Certified by the Centers for Medicare &
Medicaid Services (CMS) as a national Qualified Entity, FAIR Health
also receives data representing the experience of all individuals
enrolled in traditional Medicare Parts A, B and D, which accounts
for a separate collection of over 47 billion claim records; FAIR
Health includes among the private claims data in its database, data
on Medicare Advantage enrollees. FAIR Health can produce insightful
analytic reports and data products based on combined Medicare and
commercial claims data for government, providers, payors and other
authorized users. FAIR Health's systems for processing and storing
protected health information have earned HITRUST CSF certification
and achieved AICPA SOC 2 Type 2 compliance by meeting the rigorous
data security requirements of these standards. As a testament to
the reliability and objectivity of FAIR Health data, the data have
been incorporated in statutes and regulations around the country
and designated as the official, neutral data source for a variety
of state health programs, including workers' compensation and
personal injury protection (PIP) programs. FAIR Health data serve
as an official reference point in support of certain state balance
billing laws that protect consumers against bills for surprise
out-of-network and emergency services. FAIR Health also uses its
database to power a free consumer website available in English and
Spanish, which enables consumers to estimate and plan for their
healthcare expenditures and offers a rich educational platform on
health insurance. An English/Spanish mobile app offers the same
educational platform in a concise format and links to the cost
estimation tools. The website has been honored by the White House
Summit on Smart Disclosure, the Agency for Healthcare Research and
Quality (AHRQ), URAC, the eHealthcare Leadership Awards, appPicker,
Employee Benefit News and Kiplinger's Personal
Finance. For more information on FAIR Health, visit
fairhealth.org.
Contact:
Rachel
Kent
Executive Director of Communications and Marketing
FAIR Health
646-396-0795
rkent@fairhealth.org
1 A claim line is an individual service or
procedure listed on an insurance claim.
2 An allowed amount is the total fee paid to the
provider under an insurance plan. It includes the amount that the
health plan pays and the part the patient pays under the plan's
in-network cost-sharing provisions (e.g., copay or coinsurance if
the patient has met the deductible).
3 CPT © 2023 American Medical Association (AMA).
All rights reserved.
 View original content to download
multimedia:https://www.prnewswire.com/news-releases/mental-health-conditions-the-top-telehealth-diagnostic-category-rose-in-percentage-of-telehealth-claim-lines-nationally-and-in-every-region-in-february-2024-302143011.html
View original content to download
multimedia:https://www.prnewswire.com/news-releases/mental-health-conditions-the-top-telehealth-diagnostic-category-rose-in-percentage-of-telehealth-claim-lines-nationally-and-in-every-region-in-february-2024-302143011.html
SOURCE FAIR Health