-- Combined Company Would Improve
Affordability, Quality and Consumer Choice --
Aetna (NYSE: AET) and Humana Inc. (NYSE: HUM) today announced
plans to vigorously defend the companies’ pending merger in
response to a U.S. Department of Justice (DOJ) lawsuit seeking to
block the transaction. A combined company is in the best interest
of consumers, particularly seniors seeking affordable, high-quality
Medicare Advantage (MA) plans.
This Smart News Release features multimedia.
View the full release here:
http://www.businesswire.com/news/home/20160721005832/en/
The Aetna-Humana transaction offers tremendous value to
consumers:
- More Medicare options will be
available in more regions. Aetna and Humana will be able to
expand their offerings to more geographies, creating more options
for consumers.
- These options will offer greater
quality. Aetna and Humana have the greatest number of Medicare
Advantage plans rated four stars and higher, and will bring their
best practices together.
- These options will cost less. By
making health care more efficient and effective, Aetna and Humana
will eliminate waste and decrease costs for members.
- These options will come with new
products, tools and services that consumers want – and need.
Together, we have the team, talent and technology to develop
customized products, tools and services that deliver a better
experience.
The facts do not support the basis for DOJ action:
- There is robust competition in
Medicare. Approximately 70 percent of Medicare beneficiaries
elect to participate in traditional Medicare, administered by the
government, and that option competes with MA plans administered by
companies like Aetna and Humana. Seniors can choose from, or switch
between, traditional Medicare and an MA plan every year, or change
from one MA plan to another; data show many take advantage of these
options. A combined company would serve only 8 percent of total
Medicare beneficiaries.
- Within MA, there is an abundance of
choice for seniors, and built-in protections. In fact, 178 MA
organizations offer plans, with 28 new organizations entering MA
between 2012 and 2015 alone. Ninety-one percent of Medicare
beneficiaries can choose from at least five MA options. Each of
these plans faces rigorous government regulation to protect
consumers and promote affordability.
- To date, regulators in 18 of 20
states where change of control applications are required have
approved the transaction, with remaining reviews underway. This
is telling, because health care is delivered locally.
- Any perceived competition concerns
can be addressed through divestitures. Though the companies do
not believe divestitures are necessary, significant and
well-established industry players have already submitted bids for
MA assets in certain states that regulators may require to be
divested. Such sales would lead to alternative offerings or new
entrants in these areas, protecting competition and consumer
choice.
A combined company will result in a broader choice of products,
access to higher quality and more affordable care, and a better
overall experience for consumers. Aetna and Humana look forward to
making this clear in court, where a judge will review the
transaction based on its merits.
For more information on the competitive dynamics of traditional
Medicare and Medicare Advantage, visit
http://www.aetnaandhumana.com/wp-
content/uploads/2016/07/Medicare_MA_Competitive-R5-7-16.pdf.
For more information on the overall benefits of a combined
Aetna-Humana, visit
http://www.aetnaandhumana.com/why-were-combining/building-a-healthier-world/.
About Aetna
Aetna is one of the nation's leading diversified health care
benefits companies, serving an estimated 46.5 million people with
information and resources to help them make better informed
decisions about their health care. Aetna offers a broad range of
traditional, voluntary and consumer-directed health insurance
products and related services, including medical, pharmacy, dental,
behavioral health, group life and disability plans, and medical
management capabilities, Medicaid health care management services,
workers' compensation administrative services and health
information technology products and services. Aetna's customers
include employer groups, individuals, college students, part-time
and hourly workers, health plans, health care providers,
governmental units, government-sponsored plans, labor groups and
expatriates. For more information, see www.aetna.com and learn
about how Aetna is helping to build a healthier world.
@AetnaNews
About Humana
Humana Inc., headquartered in Louisville, Ky., is a leading
health and well-being company focused on making it easy for people
to achieve their best health with clinical excellence through
coordinated care. The company’s strategy integrates care delivery,
the member experience, and clinical and consumer insights to
encourage engagement, behavior change, proactive clinical outreach
and wellness for the millions of people we serve across the
country.
Cautionary Statement; Additional Information
Certain information in this press release regarding Aetna Inc.
(“Aetna”) and/or Humana Inc. (“Humana”) is forward- looking,
including Aetna’s and Humana’s anticipated actions regarding the
pending DOJ litigation; the impact of Aetna’s proposed acquisition
of Humana (the “Transaction”) on consumers, particularly those who
purchase Medicare Advantage Plans; a combined company’s
post-closing membership; the impact any divestitures on competition
in any geography; the anticipated benefits of a combined company
following the completion of the Transaction; and the other
anticipated benefits of the transaction. Forward-looking
information is based on management’s estimates, assumptions and
projections, and is subject to significant uncertainties and other
factors, many of which are beyond Aetna’s and/or Humana’s control.
Important risk factors could cause actual future results and other
future events to differ materially from those currently estimated
by management, including, but not limited to: the outcome of the
pending litigation in which the DOJ is seeking to block the
Transaction; the timing to consummate the Transaction if it is not
blocked; the terms and timing of any divestitures undertaken to
obtain required regulatory approvals; the risk that a condition to
closing of the Transaction may not be satisfied or that the closing
of the Transaction otherwise does not occur; the risk that a
regulatory approval that may be required for the Transaction is
delayed, is not obtained or is obtained subject to conditions that
are not anticipated; the outcome of various litigation matters
related to the Transaction that are in addition to the pending DOJ
litigation; the diversion of management time on transaction-related
issues (including the pending DOJ litigation); unanticipated
increases in medical costs (including increased intensity or
medical utilization as a result of flu or otherwise; changes in
membership mix to higher cost or lower-premium products or
membership adverse selection; medical cost increases resulting from
unfavorable changes in contracting or re- contracting with
providers (including as a result of provider consolidation and/or
integration); and increased pharmacy costs (including in Aetna’s
and/or Humana’s health insurance exchange products)); the
profitability of Aetna’s and Humana’s public health insurance
exchange products, where membership (particularly members who join
during special election periods) may have more adverse health
status and/or higher medical benefit utilization than Aetna and/or
Humana projected; uncertainty related to Aetna’s and Humana’s
accruals for health care reform’s reinsurance, risk adjustment and
risk corridor programs (“3R’s”); uncertainty related to the funding
for and final reconciliations with respect to health care reform's
risk management and subsidy programs; the implementation of health
care reform legislation, including collection of health care reform
fees, assessments and taxes through increased premiums; adverse
legislative, regulatory and/or judicial changes to or
interpretations of existing health care reform legislation and/or
regulations (including those relating to minimum medical loss ratio
(“MLR”) rebates); the implementation of health insurance exchanges;
Aetna’s and Humana’s ability to offset Medicare Advantage and PDP
rate pressures; and changes in Aetna’s and Humana’s future cash
requirements, capital requirements, results of operations,
financial condition and/or cash flows. Health care reform will
continue to significantly impact Aetna’s and Humana’s business
operations and financial results, including Aetna’s and Humana’s
pricing and medical benefit ratios. Key components of the
legislation will continue to be phased in through 2020, and Aetna
and Humana will be required to dedicate material resources and
incur material expenses during 2016 to implement health care
reform. Significant parts of the legislation, including aspects of
public health insurance exchanges, nondiscrimination requirements,
reinsurance, risk corridor and risk adjustment, continue to evolve
through the promulgation of regulations and guidance at the federal
level. In addition, pending efforts in the U.S. Congress to amend
or restrict funding for various aspects of health care reform and
pending litigation challenging aspects of the law continue to
create additional uncertainty about the ultimate impact of health
care reform. As a result, many of the impacts of health care reform
will not be known for the next several years. Other important risk
factors include: adverse changes in health care reform and/or other
federal or state government policies or regulations as a result of
health care reform or otherwise (including legislative, judicial or
regulatory measures that would affect Aetna’s and/or Humana’s
business model, restrict funding for or amend various aspects of
health care reform, limit Aetna’s and/or Humana’s ability to price
for the risk it assumes and/or reflect reasonable costs or profits
in its pricing, such as mandated minimum medical benefit ratios, or
eliminate or reduce ERISA pre-emption of state laws (increasing
Aetna’s and/or Humana’s potential litigation exposure)); adverse
and less predictable economic conditions in the U.S. and abroad
(including unanticipated levels of, or increases in the rate of,
unemployment); reputational or financial issues arising from
Aetna’s and/or Humana’s social media activities, data security
breaches, other cybersecurity risks or other causes; Aetna’s
ability to diversify Aetna’s sources of revenue and earnings
(including by developing, operating and expanding Aetna's consumer
business and expanding Aetna’s foreign operations), transform
Aetna’s business model, develop new products and optimize Aetna’s
business platforms; the success of Aetna’s Healthagen® (including
Accountable Care Solutions and health information technology)
initiatives; adverse changes in size, product or geographic mix or
medical cost experience of membership; managing executive
succession and key talent retention, recruitment and development;
failure to achieve and/or delays in achieving desired rate
increases and/or profitable membership growth due to regulatory
review or other regulatory restrictions, the difficult economy
and/or significant competition, especially in key geographic areas
where membership is concentrated, including successful protests of
business awarded to Aetna and/or Humana; failure to adequately
implement health care reform; the outcome of various litigation and
regulatory matters, including audits, challenges to Aetna’s and/or
Humana’s minimum MLR rebate methodology and/or reports, guaranty
fund assessments, intellectual property litigation and litigation
concerning, and ongoing reviews by various regulatory authorities
of, certain of Aetna’s and/or Humana’s payment practices with
respect to out-of-network providers, other providers and/or life
insurance policies; Aetna’s ability to integrate, simplify, and
enhance Aetna’s existing products, processes and information
technology systems and platforms to keep pace with changing
customer and regulatory needs; Aetna’s ability to successfully
integrate Aetna’s businesses (including Humana, Coventry, bswift
LLC and other businesses Aetna may acquire in the future) and
implement multiple strategic and operational initiatives
simultaneously; Aetna’s and/or Humana’s ability to manage health
care and other benefit costs; adverse program, pricing, funding or
audit actions by federal or state government payors, including as a
result of sequestration and/or curtailment or elimination of the
Centers for Medicare & Medicaid Services’ star rating bonus
payments; Aetna’s ability to reduce administrative expenses while
maintaining targeted levels of service and operating performance;
failure by a service provider to meet its obligations to Aetna or
Humana; Aetna’s and Humana’s ability to develop and maintain
relationships (including collaborative risk-sharing agreements)
with providers while taking actions to reduce medical costs and/or
expand the services each company offers; Aetna’s ability to
demonstrate that Aetna’s products and processes lead to access to
quality affordable care by Aetna’s members; Aetna’s and/or Humana’s
ability to maintain their relationships with third-party brokers,
consultants and agents who sell their products; increases in
medical costs or Group Insurance claims resulting from any
epidemics, acts of terrorism or other extreme events; changes in
medical cost estimates due to the necessary extensive judgment that
is used in the medical cost estimation process, the considerable
variability inherent in such estimates, and the sensitivity of such
estimates to changes in medical claims payment patterns and changes
in medical cost trends; a downgrade in Aetna’s financial ratings;
and adverse impacts from any failure to raise the U.S. Federal
government’s debt ceiling or any sustained U.S. Federal government
shut down. For more discussion of important risk factors that may
materially affect Aetna, please see the risk factors contained in
Aetna’s 2015 Annual Report on Form 10-K (“Aetna’s 2015 Annual
Report”) and Aetna’s Quarterly Report on Form 10-Q for the quarter
ended March 31, 2016 (“Aetna’s Quarterly Report”), each on file
with the Securities and Exchange Commission ("SEC"). For more
discussion of important risk factors that may materially affect
Humana, please see the risk factors contained in Humana’s 2015
Annual Report on Form 10-K (“Humana’s 2015 Annual Report”) and
Humana’s Current Reports on Form 8-K filed or furnished during
2016, each on file with the SEC. You should also read Aetna’s 2015
Annual Report and Aetna’s Quarterly Report for a discussion of
Aetna’s historical results of operations and financial condition.
You should also read Humana’s 2015 Annual Report and Humana’s
Quarterly Report on Form 10-Q for the quarter ended March 31, 2016,
each on file with the SEC, for a discussion of Humana’s historical
results of operations and financial condition. Neither Aetna nor
Humana assumes any duty to update or revise forward-looking
statements for any reason, whether as a result of new information,
future events or otherwise.
View source
version on businesswire.com: http://www.businesswire.com/news/home/20160721005832/en/
AetnaMedia Contact:T.J. Crawford,
212-457-0583crawfordt2@aetna.comorInvestor Contact:Joe
Krocheski, 860-273-0896krocheskij@aetna.comorHumana Inc.Media
Contact:Tom Noland,
502-580-3674tnoland@humana.comorInvestor
Contact:Regina Nethery, 502-580-3644rnethery@humana.com
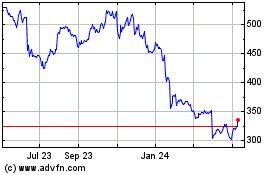
Humana (NYSE:HUM)
Historical Stock Chart
From Jun 2024 to Jul 2024
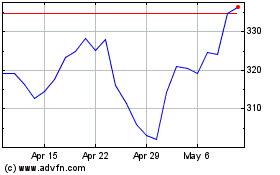
Humana (NYSE:HUM)
Historical Stock Chart
From Jul 2023 to Jul 2024